Pathophysiology - Unit 2
Syllabus
Cardiovascular System:
Hypertension, congestive heart failure, ischemic heart disease (angina,myocardial infarction, atherosclerosis and arteriosclerosis)
Respiratory system: Asthma, Chronic obstructive airways diseases.
Renal system: Acute and chronic renal failure
Scroll to Download
PATHOPHYSIOLOGY
UNIT-2
SYLLABUS
- Cardiovascular System: Hypertension, congestive heart failure, Ischemic heart disease (Angina, Myocardial infarction) Atherosclerosis (Arteriosclerosis)
- Respiratory system: Asthma, COPD.
- Renal system: Acute and chronic renal failure.
CARDIOVASCULER S.
- The cardiovascular system is composed of heart, blood vessels and blood which circulates the blood to all over the body to supply , nutrients, hormones etc.
- It is made up with two words:
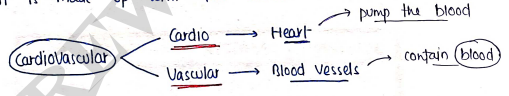
Heart : It is roughly cone-shaped hollow muscular organ, which pump blood throughout the body through blood vessels.
Blood vessels : It transports the blood to all over the body.

HYPERTENSION
- It is also known as High blood Pressure (high BP).
- Hypertension is a condition, in which pressure exerted by blood on the internal wall (lumen) of blood vessels is higher than normal.
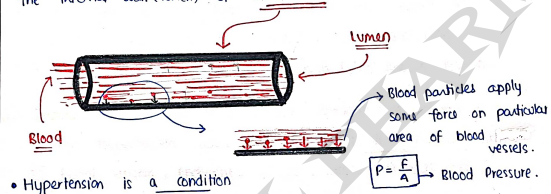
- Hypertension is a condition of elevated blood pressure for prolong period of time.
- Normal Blood Pressure =
STAGES OF HYPERTENSION
| CATEGORY/STAGES | SYSTOLIC | DIASTOLIC | |
|---|---|---|---|
| Normal | Less than 120 | less than 80 | |
| Pre-Hypertension / Elevated | 120-139 | 80-89 | starting, Just check regularly (monitoring) |
| Hypertension Stage I | 140-159 | 90-99 | immediate treatment, lifestyle changes... |
| Hypertension Stage II | 160-179 | 100-109 | |
| Hypertensive Crisis |
- It is severe condition lead to heart stroke. In this, blood vessels get damaged and heart fails to pump blood effectively to the body.
TYPES OF HYPERTENSION
On the basis of causes, it is of two types:-
- Primary Hypertension
- Secondary Hypertension
1. Primary Hypertension: Also known as Essential hypertension.
- It is most common type of hypertension about 90-95% cases of Hypertension is primary/essential hypertension.
- In this type, the cause is unidentified/no known reason.
2. Secondary Hypertension: It is less common type around 5-10%.
- In this hypertension causes due to other disease/known reason. Renal system, Endocrine, Tumors, Cardiac disorders etc.
ETIOLOGY OF HYPERTENSION
- These are causes of hypertension, there are several causes behind high blood pressure.
- It can occurs due to vasoconstriction and increases blood volume (discuss later in pathogenesis part).
- It occurs due to problem in any system:
- Renal system (kidney problem)
- Endocrine system
- Cardiovascular system
- Neurological conditions etc....
- There are various Risk factors which can cause hypertension:
- Old Age
- Obesity
- intake
- Smoking
- Alcohol
- Physical exercise
- Stress
- Family history (genetic)
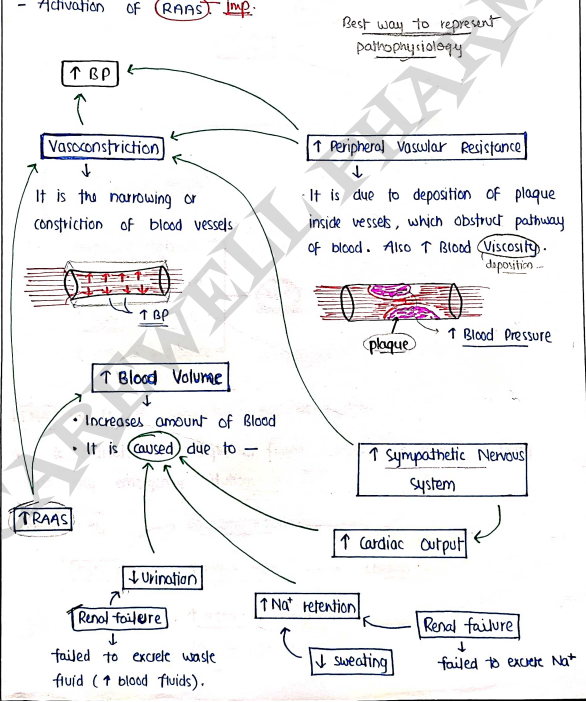
PATHOGENESIS OF HYPERTENSION
- It is the mechanism of hypertension. It is multifactorial & complex.
- It starts with several conditions:-
- Vasoconstriction and Blood volume
- peripheral vascular resistance
- Activation of sympathetic Nervous system.
- Activation of RAAS Imp.
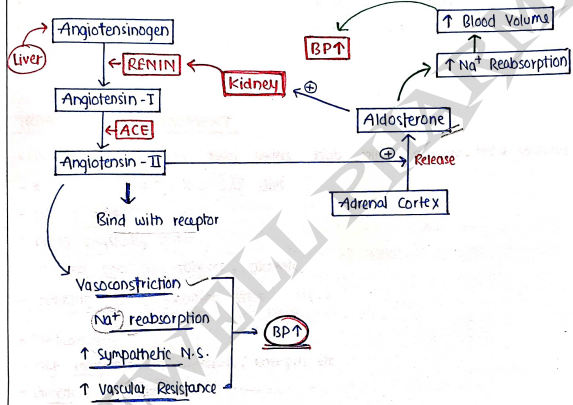
RAAS
- It is Renin Angiotensin Aldosterone System.
- It is activated when kidney/Renal perfusion decrease or kidney get low blood, then kidney release renin.
- firstly Angiotensinogen get from Liver.
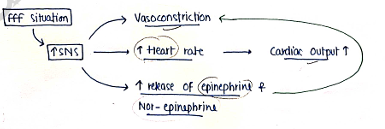
SNS
- It is sympathetic Nervous System.
- It is activated at fight or flight condition or when our body face any emergency sitution.
SIGN & SYMPTOMS
- Blurred Vision
- Chest Pain
- Headache
- Shortness of breath
- Confusion
- Fatigue
- Irregular heart beat
HYPERTENSION COMPLICATIONS
- Vision Loss
- Heart Failure
TREATMENT/MANAGEMENT
- Lifestyle changes can help lowers high blood pressure. these includes -
- eating a healthy, low-salt diet
- loosing weight
- being physically active
- quitting smoking, tobacco, alcohols.
- reducing and managing stress etc..
- Medicaments:
- ACE inhibitors. eg. Captopril, Enalopril etc.
- Diuretics. eg. thiazide etc.
- Beta blockers. eg. Atenolol, Metoprolol etc..
- channel blockers. eg. Amlodipine, Nifedipin etc.
- Vasodilators. eg Sodium nitroprusside, Minoxidil etc..
CONGESTIVE HEART FAILURE.
- It is CHF or Congestive Heart failure which is also known as Heart failure.
- It is a progressive condition in which Heart fails to pump blood in a sufficient amount to fulfil the body requirements.
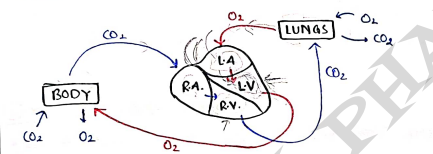
- The main work of heart is to pump the oxygenated blood to all over the body.
- In CHF, Heart fails to perform his work.
TYPES OF CHF
It is basically of two types:-
- Left sided heart failure
- Right sided heart failure
1. Left-sided heart failure:
- It is most common type in which left ventricles does not pump blood properly.
- Due to this, fluid back up in the lungs and causes shortness of breath.
- Systolic Heart failure: Left ventricle fails to contract due to reduced force of contraction. A pumping problem. After load , S.V. , C.O.
- Diastolic Heart failure: Left ventricle fails to relax due to muscles stiffness. No relaxation, no filling. A filling problem. Preload , S.V. , C.O.
Right-sided Heart failure:
- In this Right ventricles does not pump blood properly into lungs.
- Blood back-up in abdomen, legs, feet and other vital organs causing swelling.
ETIOLOGY OF CHF
It is caused due to:
- Abnormality in cardiac structure, functions, conduction, rhythm
- Hypertension or myocardial infarction
- Coronary artery disease
- Endocarditis (infection in heart valve)
- Myocarditis (infection in heart muscles)
- Cardiomyopathy (disease of heart muscles).
Some risk factors, which may increases the chance of CHF:
- High BP
- Alcohol
- High Cholesterol
- family history
- Diabetes
- Viral infection
- Smoking
PATHOGENESIS OF CHF
- It starts with any of various etiology factors.
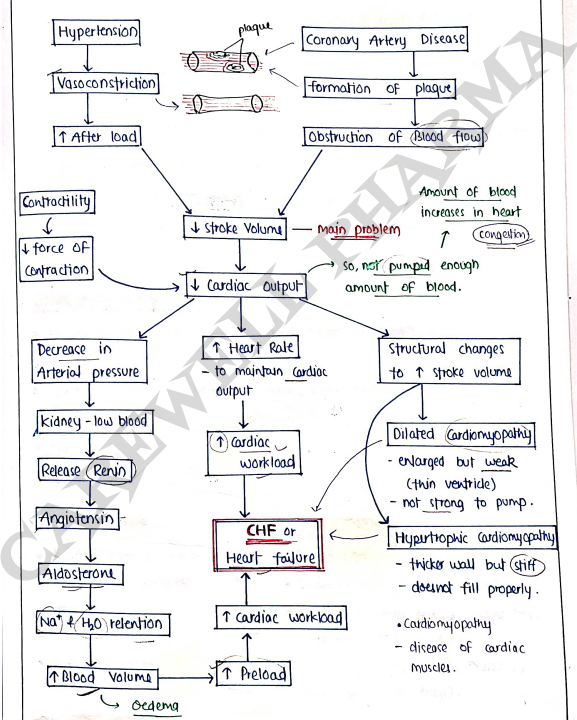
Cardiac Output It is the volume of blood pumped through left ventricle per minute. Cardiac Output (C.O.) = Stroke Volume (SV) Heart Rate (HR)
Stroke Volume It is the amount of blood pumped by the left ventricle in one beat.
Heart Rate It is the no. of times the heart beats per min. (bpm).
Preload Volume of blood that enters the left ventricles.
Afterload It is the pressure/stress in left ventricle during ejection. It represents vascular resistance & wall tension.
SIGN AND SYMPTOMS CHF
- Shortness of breath (due to accumulation of fluids).
- fatigue
- Swelling (oedema) swelling of ankles, legs, abdomen etc...
- Irregular heartbeat
- Pain in the chest
- Dizziness, Nausea etc--
COMPLICATIONS
- kidney Damage/failure
- Heart Valve problems
- Arrhythmias
- Liver damage
- Lungs disorders
TREATMENT
- Device (Artificial pacemaker)
- Surgery (bypass coronary artery)
- Self care (physical exercise, weight loss, smoking, low diet)
- Drugs (Ionotropic agents, Diuretics, Antihypertensive drugs).
ISCHEMIC HEART DISEASE
- It is a condition when our heart does not get proper amount of blood and due to damaged or diseased coronary artery.
- Coronary artery are the major blood vessels which supply the blood, oxygen and nutrients to the heart.
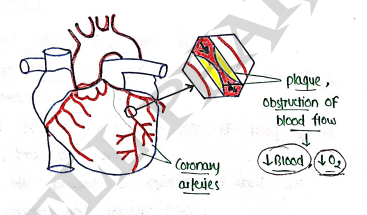
ETIOLOGY
It is caused due to coronary artery disease i.e., accumulation of plaque (atheroma) in arteries which narrow vessels & decrease blood & supply.
plaque deposition of cholesterol & other cellular waste.
It can be caused due to
- Smoking
- High blood pressure
- High cholesterol
- Diabetes
- Unhealthy lifestyle
Ischemic heart disease is further cause or responsible for:
- Angina pectoris
- Myocardial infarction
- Atherosclerosis
- Arteriosclerosis
ANGINA PECTORIS
- It is also called as Ischemic chest pain.
- Angina is severe chest pain due to ischemia (lack of to the heart muscles).
- This pain occurs in chest and left side of body spread to neck, Jaw, back and arms.
- This pain feels like pressure or squeezing in chest and this is severe, sudden and pressing pain.
ETIOLOGY OF ANGINA
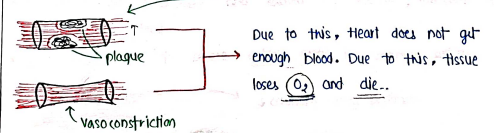
- Angina is caused when our heart muscles (myocardium) does not get enough blood and Oxygen supply.
- It is caused due to less supply or heart required more .
- It is caused due to coronary Artery Disease and vasospasm of coronary artery.
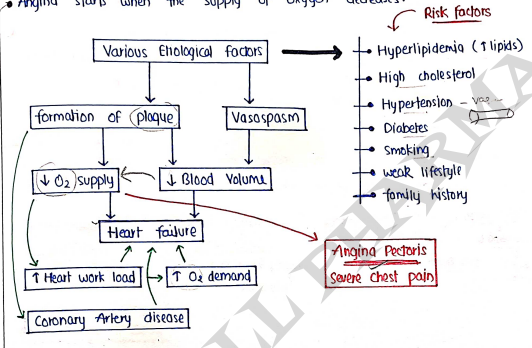
PATHOGENESIS OF ANGINA
- Angina starts when the supply of Oxygen decreases.
TYPES OF ANGINA
It is of three types:
- Stable Angina
- Varient Angina
- Unstable Angina
1. Stable Angina
- It is also known as Classical Angina and most common type of Angina.
- this Angina are predictable and caused by exercise, emotions and increased work load.
- It is caused due to severe arteriosclerotic in coronary artery.
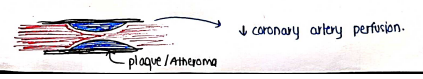
2. Varient Angina
- It is also known as Vasospastic and prinzmetal angina.
- It is uncommon and unpredictable, which occurs at rest and caused by coronary vasospasm.
- It decreases blood supply and .

3. Unstable Angina
- It occurs during rest, in this rapture of plaque happened which forms blood clot which further blocks artery and blood supply.

SIGN & SYMPTOMS
- Ischemic chest pain (spread to left side of body)
- Weakness
- Cramping
- Indigestion
- Heartburn
- Shortness of breath
- Nausea
TREATMENTS
- Self Care - Physical exercise, Weight loss + smoking.
- Surgery - Coronary artery bypass surgery.
- Drugs - Anti-Anginal drugs. Vasodilators, Beta blockers, channel blockers etc...
COMPLICATIONS
- Heart stroke or Heart Attack
- Heart failure.
MYOCARDIAL INFARCTION (MI)
- It is a condition of death of cardiac tissue due to disturbed/Obstructed blood supply to the heart.
- This is known as Myocardial infarction, or Heart Attack.
ETIOLOGY
- It is caused due to prolonged ischemia (lack of oxygen), which ultimately cause the irreversible death of heart cells.
- It is commonly caused by rapture of an atherosclerotic plaque, coronary vasospasm, Arteritis, Hypoxia etc..
PATHOGENESIS
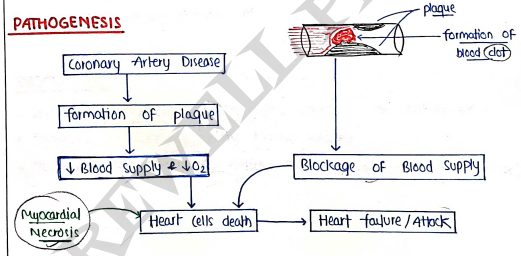
SIGN & SYMPTOMS
- Sudden chest pain
- Shortness of breath
- Anxiety
- Sweating
- Nausea & vomiting
COMPLICATIONS
- Abnormal heart rhythms
- Heart failure
- Heart Rapture
- Valve problems
TYPES OF MI
It is of two types:
- Transmural MI
- Non-transmural MI
1. Transmural MI
- In this, heart muscles undergoes ischemic necrosis which extends from endocardium to all over heart.
- It is the complete blockage of coronary artery.
2. Non-transmural MI
- In this, necrosis is extends from endocardium to myocardium. It is the partial blockage of coronary artery.
TREATMENTS
- SELF CARE Exercise, Healthy diet, weight loss, no smoking etc..
- SURGERY Coronary Artery bypass surgery
- MEDICATIONS Antianginal, Anticoagulants, Betablockers, ACE inhibitors etc...
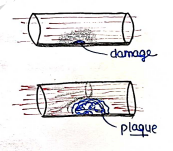
ATHEROSLEROSIS
- It is one type of arteriosclerosis, which occurs due to hardening of arteries.
- Atherosclerosis is a condition when fats, cholesterol and other waste substances are deposits in the innermost layer of artery and leads to the formation of plaque (atheroma) which further cause heart disease. (Heart attack, angina, myocardial infarction).
ETIOLOGY
- It is mainly caused due to increased level of cholesterol, fats and lipids.
- It occured:
- High cholesterol
- Obesity
- Smoking & Alcohols
- Being stressed
- Diet (excessive fat)
- Unhealthy lifestyle
- Diabetes
- Heredity
- Age
- Sex (mostly in man).
PATHOGENESIS
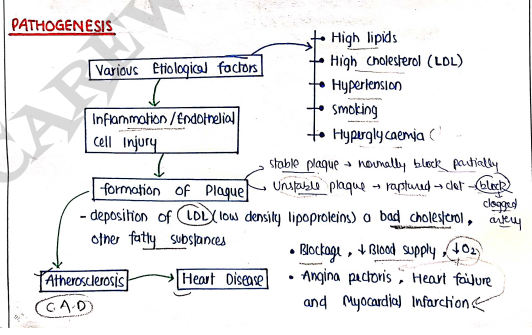
SIGN & SYMPTOMS
- Angina
- weakness & numbness of arms or legs
- Vision loss in one eye
- Hypertension
- shortness of breathe
COMPLICATIONS
- Coronary artery disease
- Heart Attack/failure
- kidney failure
- Aneurysms
TREATMENT
- SELF CARE Exercise, weight loss, low fat diet, No tobacco/Alcohol
- Medications Anticoagulants, Betablockers.
ARTERIOSCLEROSIS
- It is a condition in which the artery wall thickens (hardening of arteries) and narrow the lumen.

RESPIRATORY SYSTEM
- Respiratory system is a group of organs and tissues which help us in breathe or respiration. (exchange of gases & $CO_2$).
- The human body requires a oxygen ($O_2$) to stay alive. so, this respiratory system provides oxygen to the body's cells while removing carbon dioxide ($CO_2$) - a waste product that can be lethal if accumulated.
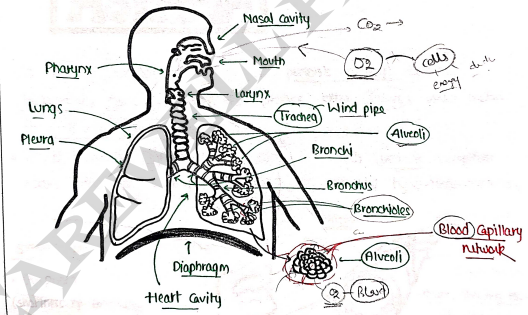
- It has three major parts:
- Airway Nasal cavity (Nose), Mouth, Pharynx, Larynx, Trachea, bronchi & bronchioles.
- Lungs main functional unit of Respiratory system, it performs O_2$/$CO_2 by alveoli. helps in breathing (inhale & exhale).
- Muscle of respiration Diaphragm, intercostal muscles in b/w cage.
MECHANISM
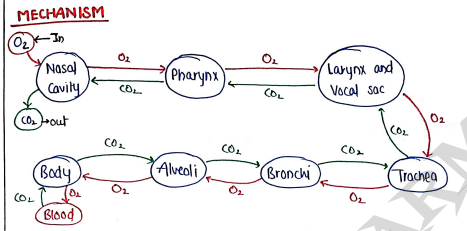
ASTHMA
- It is a condition in which a person's airway become inflammed, narrow, swell and produce extra mucus, which makes it difficult to breathe.
- It is chronic inflammatory disease in which periodic symptoms occurs due to airway obstruction and bronchial hyper-responsiveness.
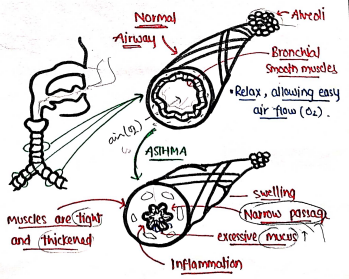
SYMPTOMS
- Dyspnoea (shortness of breathing)
- Wheezing (whistle sound during respiration)
- Cough
- Chest tightness
- fatigue
- limitation of activity.
ETIOLOGY
Asthma can be caused due to:
- Infections (lungs)
- stress
- irritants
- Anger
- Pollution (Air)
- Smoke
- Exercise
- Dust
- Exposure to cold (air)
- Pollens
- Psychogenic
- Obesity
- family history
- Chemicals/medications
TYPES OF ASTHMA
Extrinsic Asthma: It is allergic asthma. It is caused due to allergies, like dust, pollens and it also cause asthma attack. mostly episodic.
Intrinsic Asthma: It is non-allergic asthma. It is occurs due to any type of infection, stressed or cold. It is continuous.
Adult onset Asthma: more common in people younger than 40.
Occupational Asthma: affects peoples who work around chemical fumes, dust and other irritating things in the air.
Nocturnal Asthma: Get worse at night.
Drug Induced Asthma: It is caused due to medications such as Aspirin, NSAIDs, Beta-blockers etc..
PATHOGENESIS
- Asthma is an inflammatory disease, which occurs due to activation of inflammatory mediators such as mast cells, eosinophils, T-helper cells and others.
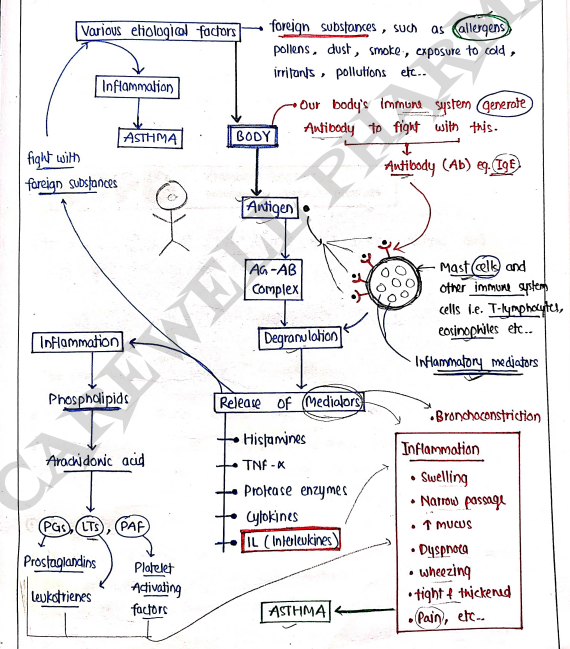
TREATMENTS
- Self care Quitting smoking and improve lifestyle.
- Oxygen therapy
- Medications Bronchodilators eg. Salbutamol, Terbutaline. Leukotriens Antagonists. eg. Montelukast, zafirlukast. Mast cell stablizers. Corticosteroids. Anti-IgE antibody.
COPD
CHRONIC OBSTRUCTIVE PULMONARY DISEASE/DISORDER
- It is a group of lung disease that blocks airflow and make it difficult to breathe.
- Chronic: for a long time
- Obstructive: Resistance/blockage
- Pulmonary: Related to lungs
- Disorder/Disease: (not reversible)
- COPD is the fourth leading cause of death.
- COPD occurs due to two most common conditions:
- Emphysema
- Chronic bronchitis
1. Emphysema
- It is a condition in which air sacs (alveoli) of the lungs get damaged, enlarged and finally burst.
- Due to this, patients/person experiences difficulty in breathing.
- It is mostly occurs due to exposure of airborne irritants/smoking.
2. Chronic Bronchitis
- It is the inflammation of the bronchial tubes, which carry and transport air.
- This condition results in formation of thick mucus, narrowing of passage, swelling which ultimately blocks the respiratory tract and make breathing difficult.
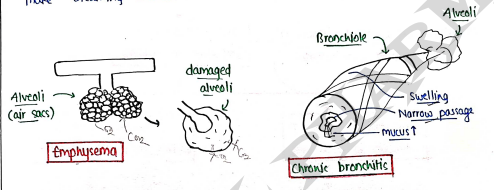
ETIOLOGY OF COPD
- Smoking (Active and Passive smoking)
- Air pollutions (irritants, allergens)
- Occupation dust/chemicals
- Airway hyper-responsiveness
- Genetic factors
- Viral infections
SYMPTOMS
- Breathing difficulty (dyspnoea)
- Cough, mucus/sputum production
- wheezing-whistle like sound
- weight loss
- fatique
- Chest tightness/pressure
COMPLICATIONS
- Lung disease/cancer
- Heart disease
PATHOGENESIS
- It mostly occurs due to emphysema and chronic bronchitis, which mainly starts from smoking.
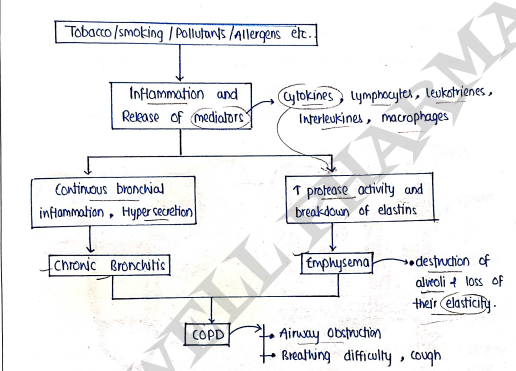
TREATMENTS
- No cure for COPD but can ease symptoms and improve quality of life.
- Self Care Physical exercise, Quitting smoking, Breathing exercise.
- Oxygen therapy provide extra oxygen to the lungs of the people with breathing difficulty.
- Medications Bronchodilators, Corticosteroids etc..
RENAL SYSTEM
- It is also known as urinary system.
- It consists of the kidney, ureters, bladder and the urethra.
- The main function of the renal system is to eliminate waste from the body (through urine), regulate blood volume and blood pressure, control levels of electrolytes and metabolites and regulate pH.
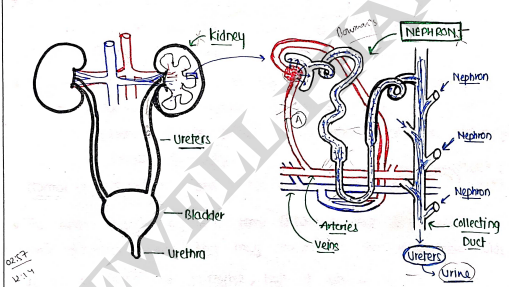
RENAL FAILURE
- It is a condition when our kidney fails to performs his work/functions.
- It is a condition, in which our kidney become unable to filter waste products from our blood.

It is of two types:
- Acute Renal failure (ARF)
- Chronic Renal failure (CRF)
ACUTE RENAL FAILURE
It is also known as Acute kidney Injury (AKI) or Acute kidney failure.
It is sudden and temporary loss of kidney/renal functions, over a period of hours, days, weeks due to loss of blood circulation in kidney or acute fall in Glomerular filtration Rate (GFR).
GFR Glomerular filtrate is the fluid that filters through the glomeruli into Bowman's Capsule and the quantity of glomerular filtrate formed in all nephrons of both kidney/min is known as GFR.
Normal (90-120) and .
- The main problem in acute renal failure is that kidneys lose their filtering ability that may accumulates the waste/toxic fluids.
- It can be fatal but reversible, but it can be turned into chronic if not treated.
ETIOLOGY
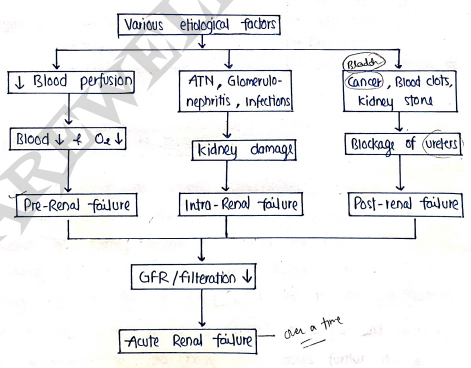
- It is of three types:
Pre-Renal ARF: It is mainly occurs due to low blood supply to the kidney. It is caused due to Blood/fluid loss ($\downarrow$ BV), Heart disease, low blood pressure, decreases Cardiac output, Liver failure, infections, and use of medications such as ibuprofen, naproxen etc..
Intra-Renal failure: It is occured due to direct damage to the structure of kidney. So, kidney not performed their work. It is caused due to Acute tubular Necrosis (ATN), blockage of veins/arteries of kidney, Glomerulonephritis (inflammation in nephrons) and due to some infections..
Post-Renal failure: It is occured due to blockage of ureters that affect the drainage/excretion of urine. It is caused due to Bladder cancer, Blood clots in urinary tract, kidney stones and prostate cancer etc..
PATHOGENESIS
- Its mechanism can be explained by its three types.
SIGN & SYMPTOMS
- Decreased urine output
- fluid retention (swelling in legs, ankles or feet)
- shortness of breath
- fatigue
- Confusion
- Chest pain/pressure etc..
COMPLICATIONS
- fluid buildup/accumulation
- Chest pain
- Muscles weakness
- Chronic Renal failure
- Death
TREATMENT
- SELF Care Avoid Some OTC medications, and Water restrictions, Make a healthy lifestyle, Avoid Risk factors.
- Medications Diuretics.
- Dialysis
CHRONIC RENAL FAILURE
- It is also known as Chronic Renal/kidney Disease.
- It is a condition of progressive or gradual loss of kidney functions and irreversible as kidney unable to filtered the blood. need dialysis & kidney transplant.
- It leads to the end stage renal disease (ESRD) in which kidney completely fails to filter blood due to damaged nephrons.
- Due to this, large amount of fluids, electrolytes and wastes are accumulated in the body which causes further disease.
- In this, GFR decreased to less than 15% (last stage).
ETIOLOGY
It is caused due to:
- Diabetes Type 1 or Type 2 diabetes ($\uparrow$ free glucose)
- Hypertension
- Glomerulonephritis (inflammation in Glomerular)
- Interstitial nephritis (inflammation in tubules)
- Polycystic kidney disease
- Vesicoureteral (urine back up) Urinary Tract
- kidney infections etc..
RISK FACTORS
- Diabetes
- Hypertension
- Smoking
- Obesity
- family
- Older age
- Use of medications / diseases
PATHOGENESIS
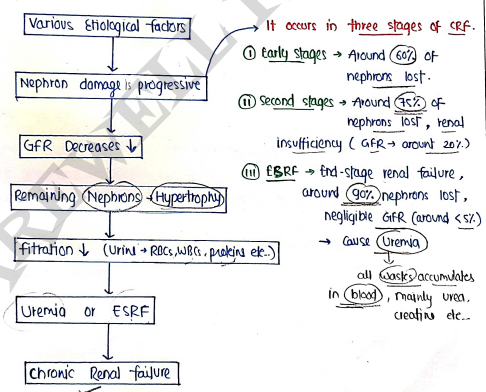
SYMPTOMS
- Nausea and vomiting
- fatigue and weakness
- Loss of appetite
- low urination/sometime more.
- Chest pain
- shortness of breath
- Erectile dysfunction
COMPLICATIONS
- fluid retention (swelling)
- Hyperkalemia ($\uparrow K^+$)
- Heart diseases
- Anemia
- Swelling (buildup of fluids)
- Muscle cramps
- Mental problem
- Hypertension etc..
TREATMENTS
- At early stages, can be manage by medicaments ACE inhibitors.
- Proper healthy lifestyle. Quit smoking, exercise, healthy Diet etc...
- At ESRF
- Dialysis (process of removing wastes, water (excess) from blood).
- kidney transplant.
