Human Anatomy And Physiology 2 - Unit 5
Syllabus
Reproductive system Anatomy of male and female reproductive system, Functions of male and female reproductive system, sex hormones, physiology of menstruation, fertilization, spermatogenesis, oogenesis, pregnancy and parturition
Introduction to genetics Chromosomes, genes and DNA, protein synthesis, genetic pattern of inheritance
Scroll to Download
REPRODUCTIVE SYSTEM
SYLLABUS
Reproductive System: Anatomy of male and female reproductive system, functions of male and female reproductive system, sex hormones, Physiology of menstruation, fertilization, spermatogenesis, Oogenesis, Pregnancy and Parturition.
Introduction to Genetics: Chromosomes, Genes and DNA, Protein synthesis, Genetic pattern of inheritance.
INTRODUCTION
- Reproductive system is one of the most important system in human body which involves the process of producing a new individual or an offspring identical to the parents.
- It involves the process of reproduction which involves the formation and transfer of gametes, fertilization, formation of zygote & embryogenesis.

It is of two types:
- Male Reproductive System
- female Reproductive system
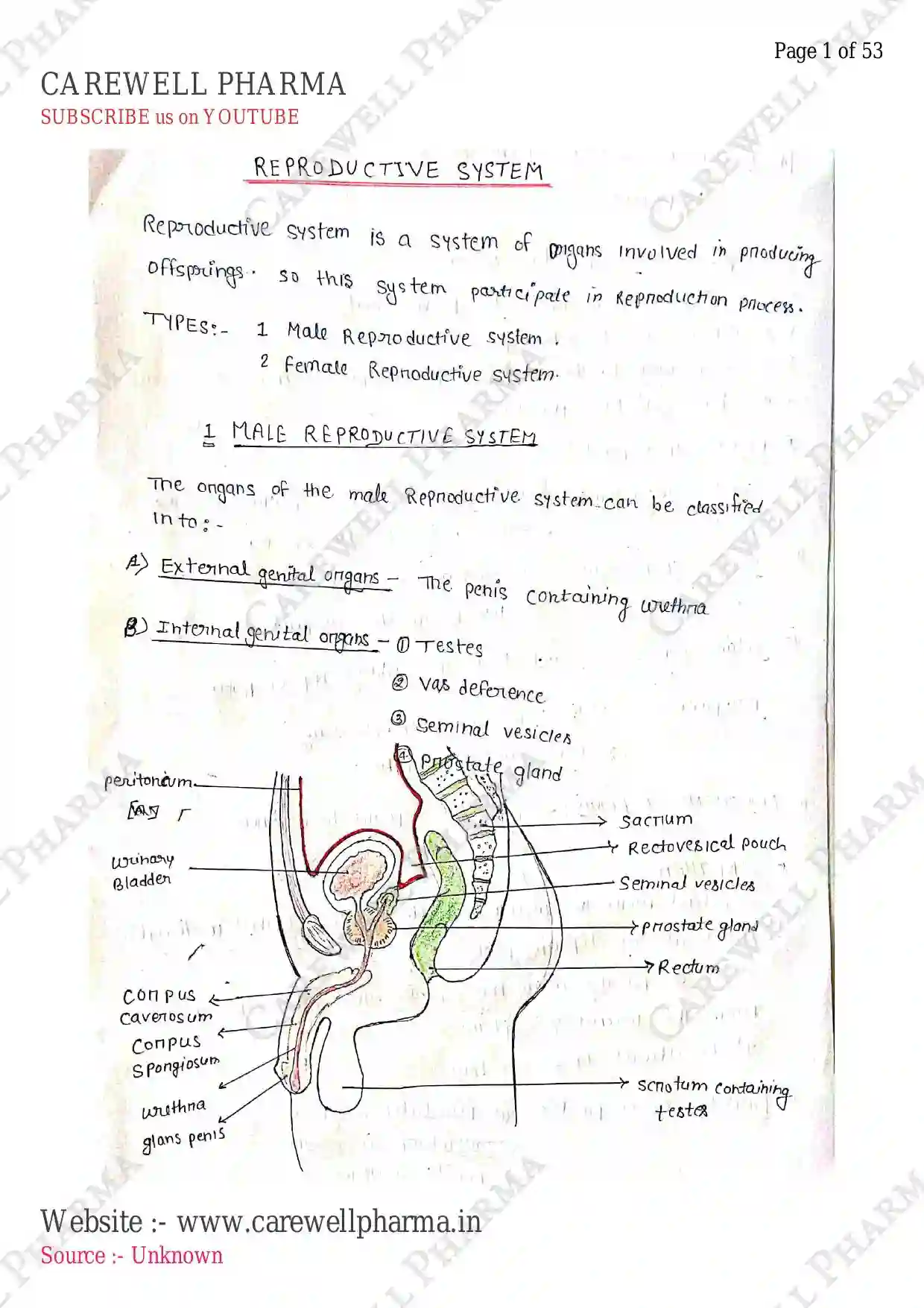
MALE REPRODUCTIVE SYSTEM
- It involves primarily in producing male gametes (sperm) and delivered it into female reproductive tract (i.e. into fallopian tube).
- It also involves the secretion of male hormones (i.e. Androgens/testosterone).
ANATOMY AND FUNCTIONS
- It is located in the pelvis region and consists of:
- a pair of testes
- Scrotum, and
- Accessory ducts
- Glands
- Penis (external genitalia)
Scrotum and Testes
- Scrotum is a pouch/sac of thick skin that protects and surrounds the testes, which are located outside the abdominal cavity.
- Scrotum helps in maintaining the low temperature of testes (i.e. lower than normal) which is required for Spermatogenesis / production of sperm.
- Scrotum has two compartment, each containing a testis, an epididymis and the testicular end of the spermatic cord.
- Testes are the oval shaped glands/bodies, around in length and wide and around in thickness.
- Testes are covered by a thick fibrous & connective tissue membrane which consists of three layer i.e. Tunica vaginalis, Tunica Albuginea, Tunica Vasculosa.
- They remain suspended in the scrotum via spermatic cords.
- Each testis contains about 200-300/250 testicular lobules/compartments. Each lobule contains 1-4 seminiferous tubules and these are lined by two types of cells:-
- Male germ cells (spermatogonia) spermatogenesis to produce sperm.
- Sertoli cells they provide nutrition to germ cells.
- Interstitial spaces is a space around the seminiferous tubules, which contains small blood vessels and interstitial/Leydig cells which secrete Andogen / testosterone.

Accessory Ducts
- Rete testis Seminiferous tubules open into vasa efferentia through rete testis.
- Vasa efferentia/efferent ductules they leave the testes and open into epididymis.
- Epididymis Each epididymis is a tube about 20 feet long, which is tightly coiled and bunched into a length of just 2 inches. Epididymis stored sperm and act as a site of sperm maturation.
- Spermatic cords The abdominal cavity is connected with the testes by two spermatic cord in the scrotum, also it contains nerves, veins, arteries, and lymphatic vessels.
- Vas deferens / Ductus deferens / deferent duct It caries the sperm in the upward direction to reach the ejaculatory duct via epididymis.
Glands
- Seminal vesicles These are paired exocrine glands present behind the urinary bladder and in front of rectum. They store and produce a liquid and fructose fraction of semen for the survival of sperm.
- Ejaculatory duct It unites the vas deferens, prostate gland secretion, with the urethra and also contain the duct of seminal vesicles. It collectively ejects semen (sperm + secretion of seminal vesicles + secretion of prostate gland).
- Prostate gland Around of the semen is made up of prostatic secretion i.e. A thin, milky fluid having pH , containing zinc, citric acid, sperm motility factors, phosphate, proteolytic enzymes (fibrinolysin) is secreted. It also secretes PSA (Prostate-Specific Antigen) in case of prostatic cancer as diagnostic factors.
- Bulbourethral / Cowper's glands It is pea-sized glands situated inferior to the prostate gland which secrete alkaline/basic mucus into duct and drain into urethra. It is used for penis lubrication, and for pH neutralisation (sperm survives better in basic than acidic medium in female vagina due to killing bacteria) for sperm motility.
External Genitalia (Penis)
- It is cylindrical-shaped, suspended below the abdominal cavity. The enlarged end of penis is called the glans penis, which is covered by a loose fold of skin called foreskin.
- It contain erectile tissue, i.e. corpora spongiosum (which covers the urethra) and corpora cavernosa (lie side by side).
- The penis becomes erect/rigid when these tissue are filled with blood.
- Helps in the erection & facilitate insemination/fertilization.

- functions -
- deposits sperm in vagina of female.
- produces pleasurable sensation during sexual activities.
FEMALE REPRODUCTIVE SYSTEM
- It involves primarily in producing female gametes (i.e. Ovum) which further fertilized when sperm fused with ovum and form zygote.
- The primary sex organs in females are a pair of ovaries which produce ova/egg and they also secrete female sex hormones like progesterone and estrogen.
ANATOMY AND PHYSIOLOGY
- It is divided into two parts:
- External Genitalia (vulva)
- Internal Genitalia Vagina, Uterus, Uterine tubes and Ovaries.

Internal Genitalia
- These are situated inside the abdominal cavity / located in pelvic region which contains:-
Vagina
- It is a muscular and elastic tube that connects the cervix to the external body.
- It is around 3 inches long and less than an inch in diameter.
- It functions as the receiver for the penis in sexual intercourse, and delivers sperm to the fallopian tubes and uterus.
- It also acts as birth canal by expanding to allow delivery of foetus during childbirth.
- It provides a passage for blood during menstruation.
Uterus
- It is also called the womb, which is present within the pelvic region between the bladder and rectum. (, , thickness $2.5 \text{ cm}$).
- It is made up of three parts:
- Fundus uppermost rounded part b/w two uterine tubes.
- Body It is the part extending from fundus to cervix.
- Cervix It is lower narrow part and connect to vagina and act as entry for uterus.
- It consists of three layers:
- Perimetrium/Peritoneum A thin outermost layer.
- Myometrium A middle thick layer.
- Endometrium A inner glandular layer, which release mucus and provides blood supply to the foetus which attached on the endometrium.
- functions It receives the fertilised ovum, feeds the foetus during pregnancy and provides nourishment. It also Involves in menstruation and childbirth.
Fallopian / uterine tubes (Oviduct)
- These are a pair of muscular tubes and funnel-shaped structure, extend from the right and left upper corners of the uterus to the edge of ovaries.
- It is around long and in diameter.
- It consist of Isthmus (closest to uterus), Ampulla (middle portion), Infundibulum contain finger-like fimbriae (which collect the ovum from ovary after ovulation).
- functions They provide the site of fertilisation, collects the ovum and send this fertilised egg to the uterus for implantation.
Ovaries
- These are oval shaped paired organs present on both side of uterus at lower abdomen in pelvis.
- functions act as the main female sex organs which produce female gamete (ovum) and secrete hormones i.e. oestrogens and progesterone.
- Each ovary is about in length which then connected to the uterus, and pelvic wall through ligaments.
- outer cortex and inner medulla.
- The ovary is surrounded by a thin covering of epithelium, encloses the ovarian stroma and divided into two zones.
- The cortex consist of various ovarian follicles (basic unit) which nurture the developing oocyte and secrete oestrogen when the follicle grows.
Breast (Mammary Glands)
- These are paired structure of glandular, fibrous and fatty tissues.
- Around 20 lobes of glandular tissue are present in each breast and each lobules surrounding the nipple.
- These lobules have a cluster of alveoli containing cells which secrete milk.

- (Alveoli) open into mammary tubules fuse to form mammary duct milk reservoirs (lactiferous sinus) Lactiferous ducts nipple (milk is sucked out).
- functions Breasts are not considered sexual but are a part of the female reproductive system. In this mammary glands produce milk to feed the baby.
External Genitalia (Vulva)
- These are external part of female reproduction system known as vulva.

- Mons Pubis is a pad of fatty tissue present over the pubic bone, covered with pubic hair after puberty.
- Labia majora are folds of hair covered skin.
- Labia minora are more pigmented, paired folds of tissue, both protects the female urethra and entry of vagina.
- Clitoris (also glans clitoris) is a small finger like structure, work as pleasure centre for female reproductive system.
- Hymen is a thin membrane, located b/w the urethral and anus, which partially covers the vaginal openings.
- Vestibular glands/vestibule is located b/w the labia minora (borders of vaginal opening) contain opening of urethra, vagina. Bartholin's glands.
SEX HORMONES
- Regulated by LH (Luteinizing hormone) and FSH (Follicle stimulating Hormone).
- These are those hormones which produced by endocrine system and play an important role in sexual development, growth, reproduction and functions of human body.
- These are of two types:-
- Male sex hormones
- female sex hormones
Male sex hormones
- These are those hormones which release from male sex organs (testes) and that helps in the development of sexual organs (growth) after Puberty and also helps in spermatogenesis (production of sperms).
- Example: Androgens, including testosterone.
- Testosterone: It is a primary male sex hormones.
- It helps in the development of male reproductive tissue such as testes and prostate.
- It promotes spermatogenesis, increased sexual characteristics such as muscles, bone mass, body hairs etc..
Female sex hormones
- These are those hormones which release from female sex organs (ovaries) and that helps in development of sexual organs (growth) and also helps in ovulation (release of ovum).
- Examples: Estrogens and Progesterons.
- Estrogen: It regulates menstrual cycle, fertility and pregnancy. maintain female sexual characteristics and bone density.
- Progesterone: It prepares uterus for pregnancy and maintains it. regulates embryogenesis and breast growth, ovulation.
- These two hormones are essential for female reproductive health and development.
PHYSIOLOGY OF MENSTRUATION / MENSTRUAL CYCLE
- The menstrual cycle is a monthly process in which a female's body prepares for a potential pregnancy, involving hormones changes, ovulation, and uterine lining (endometrium) growth, ending with menstruation (periods) if pregnancy doesn't occurs.
Menstruation
- It is the shedding of the uterine lining (endometrium) in a woman's reproductive system, typically occuring monthly if pregnancy doesn't occurs, resulting in vaginal bleeding (periods).
Menstrual Cycle

- The menstrual cycle is counted from the first day of one period to the first day of the next.
- It is not same for everyone, generally, it happened in 28 days but it vary from 21-35 days.
- This cycle is divided into four phase, which involves hormonal and physiological changes.
- Menstruation (Days 1-5) vary from (2-7 days)
- Follicular phase (Days 6-14)
- Ovulation (Day 14)
- Luteal phase (Days 15-28)
- Menarche first menstruation.
- Menopause Last menstruation (stop permanently).
1. Menstruation Phase (Days 1-5)
- It involves menstrual bleeding, in which uterus sheds its lining (endometrium) resulting in vaginal bleeding (periods).
- It is due to decreasing level of estrogen and progesteron.
- In this phase, Cervix produce mucus which help to flush out the uterus.
2. Follicular phase (Days 6-14)

- It involves the development of multiple follicles in the ovaries, fluid filled sac, contains eggs. Stimulated by FSH (follicle-stimulating hormone).
- one follicle becomes dominat, which is choosen for ovulation (release of egg/ovum).
- Also, estrogen levels increases to thicken the uterine lining (endometrium).
3. Ovulation (Day 14) (It also can be change)
- It involves the release of egg (ovum) from the dominant follicle from ovary release into fallopian tube. The egg is viable for fertilization for 12-24 hours.
- In this, ovulation is triggered by Luteinizing hormone (LH) which is released from pituatary gland. (Sperm Active for 3-5 days, Best upto 48 hours).
4. Luteal phase (Days 15-28)
- In this, the empty follicle transforms into corpus luteum which produce progesterone.
- Now this increased level of progesterone, prepared the uterus for implantation.
- Now this uterus is receptive to implantation for 4-5 days.
- final If fertilization/pregnancy occurs, the embryo/zygote implants in the uterus. If not occurs, then the corpus luteum degenerates and progesterone levels drop/decreases which leads to menstruation.
CONCLUSION Hormonal (regulation)

- Estrogen produces in follicular phase.
- Progesterone produces in luteal phase.
- Hypothalamus Pituatary Gland LH/FSH Testes/ovaries Testosterone, Estrogen, Progesteron.
- LH/FSH releases from pituatary glands which regulates release of Estrogen / Progesteron.
- Menstruation (periods) occurs if egg not fertized, due to decreased level of progesterone / estrogen.
FERTILIZATION
- It is a process by which a sperm fertilizes an egg, resulting in the formation of a zygote.
- It is the fusion of sperm with the egg/ovum.
- fertilization occurs in the ampulla of the fallopian tube.
PROCESS
- It involves the several steps:-
- Sperm migration ($300 \text{ M}$) sperm in semen deposited in the vagina during ejaculation and enter the fallopian tube, where fertilization occurs.
- Sperm capacitation Now, sperm undergoes changes itself to become more motile and capable of fertilization (movement).
- Ovulation It involve the releasing of egg from the follicle of ovary, which enters the fallopian tube.
- fusion Now, finally sperm meets the egg in fallopian tube. Then, sperm releases enzymes from acrosome (head of sperm) (hyaluronidase) which penetrate the corona radiata, zona pellucida and reaches egg's plasma membrane then sperm fuses with egg's plasma membrane & form fertilization cone.
- Zygote Now, a single cell, the zygote is formed, which contains genetic material from both parents (sperm DNA + Egg DNA). (diploid cell).
IMPORTANT NOTE
- Egg's cortical granules release enzymes which prevent polyspermy (multiple sperm fertilization).
- Now, Zygote begins to develop & cleaved.

- fertilization depends upon:
- Sperm quality (motility, count)
- Egg quality (maturation, viability, receptivity)
- Timing (during fertile window)
- Hormonal balance (Estrogen, Progesterone, LH/FSH etc.).
After fertilization, there are several steps:
- During fertilization zygote is formed, after this zygote undergoes cleavage (rapid mitotic cell division).
- continuous cleavages of zygote result in a morula (a solid sphere of cells surrounded by the zona pellucida, almost same size as original zygote).
- After 5th day of fertilization, morula enters the uterus. After 32-cell stage, these morula form blastocyst.

- After implantation, blastocyst develops into an embryo which undergoes rapid growth and differentiation (embryogenesis, organogenesis) then this embryo develops into fetus, begining of a new individual's life.
PREGNANCY
- It is a process by which a developing fetus grows inside the female reproductive system.
- It occurs when blastocyst implants on the uterine line (endometrium), then it release Human chorionic Gonadotropin (HCG) hormone in blood and urine, which can be detected by using pregnancy kit or if period missed.
- It occurs for 40 weeks from 1st day of last menstruation to the normal childbirth, lasts for 9th months.
Various phases of pregnancy divides into three trimesters:
- first trimesters (week 1-12)
- Second trimesters (week 13-26)
- Third trimesters (week 27-40)
- Parturition/childbirth
1. first trimester (week 1-12)
- It occurs for 1-12 weeks. In this, firstly menstruation and Ovulation occurs in 1-2 week, which further follow fertilization and Implantation of zygote.
- Then this blastocyst/trophoblast forms a functional unit placenta b/w developing embryo and maternal body (mother).
- Then this embryo undergoes embryogenesis (week 3-8) (heart is formed 7-8 week) then organs formation and development start from week 9-12 (limbs, fingers, toes).
2. Second trimesters (week 13-26)
- This phase mainly involves the development of fetus.
- Organ functioning, nerve development (week 13-14), Eye, ears, nose, mouth development (week 15-16), muscle, bones (week 17-18), skin development (week 19-20), Brain & Nervous system (week 21-22), lung development, breathing (23-24), fetal growth, starts to kick, reflexes (week 25-26).
3. Third trimesters (week 27-40)
- It involves fetal maturation and preparation for birth (week 27-32).
- final fetal development and growth (week 33-36).
- preparation for Labor and delivery (week 37-40).
4. Parturition
- It is the process of childbirth, from the onset of labor to the delivery of the baby.
- Labor is the process or sign by which the uterus contracts to push the baby out of the birth canal.
Sign of labor:
- Contraction (cramping or tightening in the uterus)
- Bloody show (mucous plug release)
- rupture of membranes (water breaking)
- Back pain
- Nausea and Vomiting
It can be normal vaginal delivery. After completion of time, signal produced for parturition, which induces foetal ejection reflex which triggers the release of Oxytocin which helps in contraction and delivery of baby.
C-section and instrumental delivery for abnormal cases.
Postpartum
- Postnatal period remains for about 6 week after childbirth. Continues, even after 6 week.
- It involves the changes occurs after birth:
- physical recovery.
- Emotional changes.
- Bonding with the baby.
- Lactation and breastfeeding.
GAMETOGENESIS
- It involves the formation of gametes.
- spermatogenesis is the formation of sperms.
- oogenesis is the formation of ovum.
SPERMATOGENESIS
- It is the process by which immature cells develops into mature sperm cells. This process occurs in the seminiferous tubules of the testes and take approx. 70-80 days to complete.
STAGES OF SPERMATOGENESIS
- Spermatogonia: Immature cells that develop into sperm cell. these are diploid (46 chromosomes) and stem cells of male R.S.
- Spermatocytogenesis: spermatogonia undergoes mitosis to produce two primary spermatocytes (16-20 days). One remains in basement as stem cell and other in growth.
- Meiosis: Primary spermatocytes undergoes meiosis I (10-14 days), produce two haploid secondary spermatocytes. These undergoes meiosis II (10-14 days), produce four haploid spermatids (round cells with no tail).
- Spermiogenesis: Spermatids converts into mature sperm (10-15 days) in (epididymis), in which sperm fully developes.
HORMONAL REGULATION
- FSH (follicle-stimulating hormone): stimulates spermatogonia to undergo mitosis.
- LH (luteinizing hormone): stimulates the production of testosterone. essential for development & maturation of sperm cells.


Spermiogenesis
- Divided into three regions:
- Head contains DNA and acrosome contain enzymes.
- Body contain mitochondria which provides energy to sperm to swim.
- Tail type of flagellum, which helps the sperm to move (Microtubules).
- A healthy adult male produces around 400 million sperm per day via spermatogenesis.
- Disruptions/Abnormalities in spermatogenesis can leads to infertility & Birth defects.
OOGENESIS
- It is the process of formation of egg/mature ovum.
- It is the complex process by which immature cells in the female reproductive system develop into mature egg cells (oocytes).
- This process occurs in the ovarian follicles of the ovaries and takes approx. 120-150 days to complete.
STAGES

- Immature cells (PGC - primordial gamete cells) undergo Mitotic division to form Oogonia (diploid stem cell of ovaries).
- Oogonia undergo mitosis to produce primary oocyte (Oocytes), involves replication of DNA. (Oocytogenesis).
- Oocytes undergo meiosis I and II, forms haploid cells (23 chromosomes).
- Secondary oocytes developed within Ovarian follicles releases as a mature egg cells into fallopian tubes.
NOTE
- LH stimulates Ovulation, also FSH, estrogen regulates it.
- These polar body are non-functional, only one type of oocyte is formed.
- Oogenesis begins from birth and continues till menopause.